Human mini-bladder reveals mechanism that promotes recurrent urinary tract infections
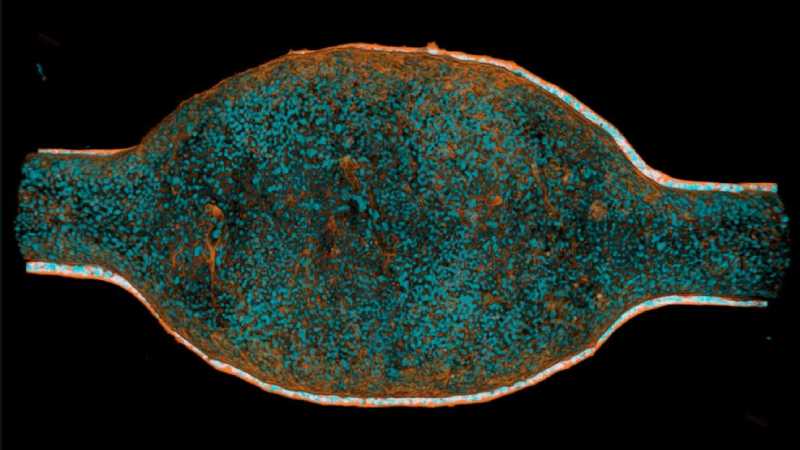
Researchers in bioengineering and human biology have developed a groundbreaking miniature human bladder model capable of reproducing the complex interactions between urine, bladder tissue, and bacteria that cause urinary tract infections (UTIs). The study, published in Nature Communications, demonstrates how the composition of urinary fluid can weaken the bladder barrier and facilitate the persistence of recurrent bacterial infections—a public health issue affecting millions of people worldwide.
The human bladder is far more than a simple urine reservoir: its mucosa, composed of a specialized layer of cells known as the urothelium, continuously interacts with urine during filling and emptying cycles. Although it is known that urine composition can vary—shaped by factors such as hydration, diet, and metabolic disorders—the way these variations influence tissue integrity and the response to bacterial infection had not been fully understood.
To explore these mechanisms in a controlled environment, scientists from EPFL, Heidelberg University, and the Roche Institute of Human Biology in Basel created a microfluidic device containing human cells organized into a multilayered structure resembling the real bladder lining. This “mini-organ” was then exposed to urine of varying compositions and infected with uropathogenic Escherichia coli (UPEC), the primary bacterium responsible for UTIs, particularly recurrent cases.
The experiments revealed that prolonged exposure to highly concentrated urine weakens the connections between urothelial cells—so-called “tight junctions.” This weakening compromises the bladder’s natural defenses, reduces the expression of genes involved in the local immune response, and facilitates bacterial invasion. In contrast, tissues exposed to less concentrated urine maintained greater resilience and preserved their protective barrier.
When the mini-bladder was infected with UPEC, the team observed that tissues exposed to highly concentrated urine accumulated more bacteria internally. In addition, the effectiveness of antibiotics such as fosfomycin—often prescribed as a first-line treatment for uncomplicated urinary tract infections—was reduced.
The surprising explanation was the formation of cell wall–deficient bacteria (CWD UPEC), abnormal forms that remain viable despite the presence of antibiotics and can lodge deep within the layers of the urothelium, serving as “reservoirs” for future infections.
These CWD UPEC not only resist the action of medications but can also reemerge and restart infection after treatment ends—a likely direct mechanism of bacterial recurrence that helps explain why some patients experience repeated infections even after seemingly effective antibiotic courses.
The study’s findings offer a new perspective on the active role of urinary composition in the development and recurrence of UTIs. The discovery that solute-rich urine can weaken the mucosa and promote bacterial survival suggests that factors such as hydration and metabolism may be just as important as antibiotic therapy itself in preventing recurrent infections.
Furthermore, the miniature human bladder model represents a powerful tool for testing new therapies and evaluating antibiotic responses in an environment that more closely replicates human physiological conditions. Previous research using three-dimensional tissue models has also indicated that a deeper understanding of interactions between pathogens and the human urothelium is crucial for advancing treatment of persistent and antibiotic-resistant UTIs.
Complementary studies have explored alternative approaches, such as intravesical therapies designed to reinforce the bladder lining or strategies aimed at modulating the genitourinary microbiome to reduce UTI frequency. However, widely effective clinical solutions for recurrent forms of the disease remain limited.
As global bacterial resistance to antibiotics continues to rise, innovations such as the miniature human bladder model may prove essential for developing more effective and personalized treatments—ones that consider not only the pathogen itself but also the physiological context in which it lives, adapts, and returns.





